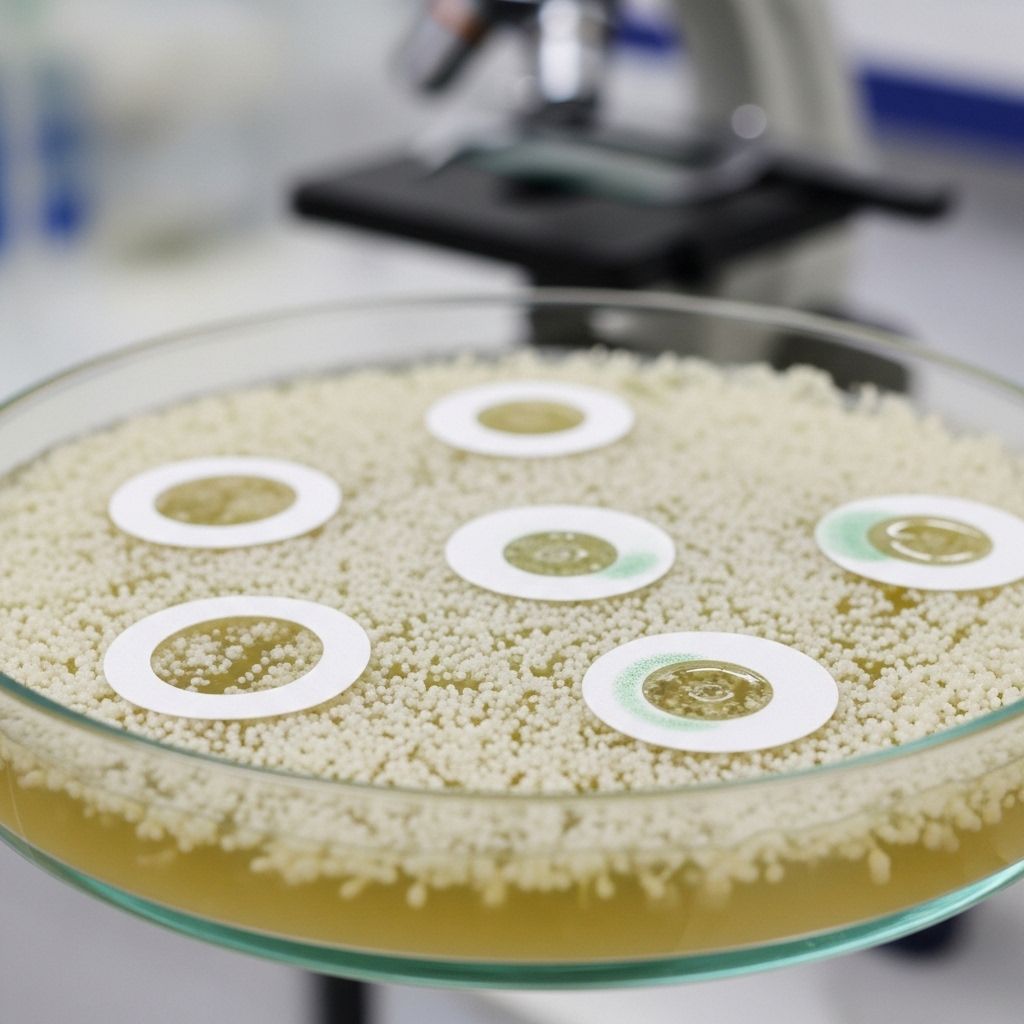
Kirby-Bauer disc diffusion testing of isolates recovered from Düsseldorf office building surfaces. Reduced inhibition zones indicate resistance phenotypes.
Why This Study Was Necessary
Antimicrobial resistance (AMR) surveillance in Germany, as in most European countries, has historically been focused almost exclusively on clinical settings — hospitals, long-term care facilities, and outpatient clinics. This focus is entirely rational given where the morbidity and mortality burden of AMR infections is concentrated. But it has created a significant blind spot in our understanding of how resistant organisms circulate and persist in the broader built environment.
A growing body of international evidence — studies from the United States, United Kingdom, Japan, and Sweden — has documented the presence of MRSA, ESBL-producing Gram-negative bacteria, and even carbapenem-resistant organisms in non-clinical built environments including offices, schools, fitness centers, and retail spaces. No comparable systematic German data set existed when this study was initiated in January 2021.
Study Population: 19 Office Complexes, Three Years of Data
Sampling was conducted quarterly across 19 commercial office complexes in Düsseldorf (11 buildings) and Frankfurt am Main (8 buildings). Buildings were selected to represent a range of occupancy densities (80–1,200 daily occupants), construction eras (1978–2019), cleaning contract types (in-house, outsourced standard, outsourced premium), and proximity to healthcare facilities (0.3 km to 4.7 km from major hospital campuses).
Each quarterly sampling round collected 48 samples per building across six surface categories: desk and keyboard surfaces, door handles and push plates, shared printer and copier touchpads, restroom touchpoints (taps, flush handles, soap dispensers), communal kitchen surfaces (refrigerator handles, microwave touchpads, coffee machine controls), and HVAC outlet grilles. Samples were processed for culture-based detection of AMR organisms and subjected to whole-genome sequencing for a representative subset of resistant isolates.
Principal Findings: A Statistically Significant Upward Trend
Across all 19 buildings and the full 36-month study period, the study documented a 34% increase in the prevalence of AMR organisms per sampled surface from Q1 2021 to Q4 2023. This trend was consistent across both cities, across all building age categories, and across all cleaning contract types — though the magnitude varied significantly by cleaning regime.
The specific organisms identified and their prevalence trends:
| Organism | Resistance Phenotype | Prevalence (Q1 2021) | Prevalence (Q4 2023) | Change |
|---|---|---|---|---|
| Staphylococcus aureus | MRSA (methicillin-resistant) | 6.2% of surfaces | 9.8% of surfaces | +58% |
| Klebsiella pneumoniae | ESBL-producing | 3.1% of surfaces | 5.4% of surfaces | +74% |
| Escherichia coli | ESBL-producing | 4.8% of surfaces | 7.2% of surfaces | +50% |
| Staphylococcus epidermidis | QAC-tolerant (qacA/B positive) | 18.3% of surfaces | 29.6% of surfaces | +62% |
| Enterococcus faecium | VRE (vancomycin-resistant) | 0.9% of surfaces | 2.1% of surfaces | +133% |
"The 133% increase in VRE prevalence is the single most alarming figure in this dataset. Vancomycin-resistant enterococci are a tier-one clinical concern — organisms for which treatment options are severely limited. Their presence and growth in ordinary commercial office spaces represents a community reservoir that has, until now, been essentially invisible to surveillance systems."
The Disinfectant Tolerance Connection
Whole-genome sequencing of representative resistant isolates revealed a striking pattern: the organisms showing the most dramatic prevalence increases — S. epidermidis QAC-tolerant strains and MRSA isolates — were those most likely to carry efflux pump gene families conferring simultaneous tolerance to the QAC-based disinfectants used in all 19 buildings' cleaning programs and reduced susceptibility to clinical antibiotics.
This is the disinfectant-resistance cross-selection phenomenon documented in laboratory settings, now observed at scale in real-world built environments over a three-year period. The routine application of QAC disinfectants — at concentrations that inactivate susceptible organisms while leaving tolerant organisms marginally affected — appears to be actively selecting for the organisms most likely to cause clinically significant infections in building occupants.
The Keyboard Paradox
The surface category showing the highest AMR organism prevalence across the study was not, as many might predict, restroom surfaces or door handles, but shared keyboard and computer input devices. Shared keyboards — common in open-plan offices, reception desks, meeting rooms, and hot-desk environments — showed MRSA prevalence rates of 12.4% in the final sampling round, compared to 7.1% for restroom door handles and 4.8% for external door handles.
The explanation lies in cleaning frequency. Restrooms and entrance fixtures are cleaned daily in most of the sampled buildings; shared keyboards are cleaned, on average, once every 6.2 weeks. The combination of high-contact frequency, low cleaning frequency, and porous key-cap surfaces that resist chemical disinfection creates an exceptionally favorable persistence niche for AMR organisms.
What Should Building Managers Do?
The study findings translate into a set of practical, actionable interventions that building management and facilities teams can implement without waiting for updated regulatory guidance:
- Diversify disinfection chemistry: Replace QAC-only disinfection programs with rotational protocols incorporating hydrogen peroxide-based compounds or alcohol-based products to reduce QAC tolerance selection pressure.
- Include input devices in cleaning schedules: Keyboards, mice, and touchpad devices should be cleaned with viricidal/bactericidal wipes at weekly minimum frequency; daily in hot-desk environments.
- Establish baseline AMR surveillance: Annual microbiological assessment of office surfaces using targeted AMR screening (not merely generic microbial counts) provides the data required for evidence-based cleaning protocol adjustment.
- Engineer out high-contact touchpoints: Automatic soap dispensers, touchless faucets, automatic lighting, and sensor-activated doors reduce cumulative surface-contact frequency significantly.
- Review cleaning contract specifications: Ensure cleaning service specifications include minimum contact time requirements for disinfectants (most QAC-based products require 30–60 seconds of surface wetness to achieve label-claimed efficacy; rushed cleaning operations routinely fail to meet this requirement).
Sources & References
- Braun F, et al. Longitudinal surveillance of antimicrobial-resistant organisms in German commercial office environments 2021–2023. CleaningHouses Research Series, 2024.
- European Centre for Disease Prevention and Control. Antimicrobial resistance in the EU/EEA: A One Health response. ECDC Annual Report, 2023.
- Linfield R, et al. Environmental persistence and transmission of community-acquired MRSA in non-healthcare settings. Infection Control and Hospital Epidemiology, 2021;42(5):541–548.
- Kampf G. Biocidal agents used for disinfection can enhance antibiotic resistance in gram-negative species. GMS Hygiene and Infection Control, 2018;13:Doc11.
- Robert Koch Institute. Empfehlungen zur Prävention und Kontrolle von MRSA-Stämmen. Bundesgesundheitsblatt, 2023;66(2):217–230.
About the Author
Dr. Felix Braun
Clinical microbiologist and environmental health researcher. Senior contributor to CleaningHouses on antibiotic resistance and built-environment AMR dynamics.